Chief Complaint: 68-year-old male with decreased vision, OD.
History of Present Illness: Patient has noticed a three day history of decreased visual acuity OD, right periorbital headache, and right periorbital rash.
Ocular History: No previous ocular history. No eye surgery, trauma, nor contact lens use.
Medical History: History of basal cell cancer of the nose. Review of systems was otherwise negative.
Medications: None
Family History: Noncontributory
Social History: Noncontributory
EXAM OCULAR
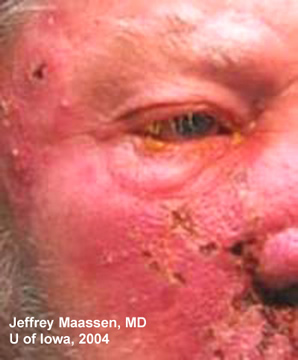
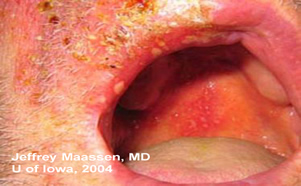
| A: Crusted, vesicular lesions in the V2 distribution, limited to the right side/respecting the midline. Ectropion noted temporally secondary to edema/induration infraorbitally. | B: Crops of vessicular lesions in V2 distribution well delineated on upper lip and oropharynx. |
 |
 |
Discussion:
Herpes zoster occurs after primary infection with the zoster virus. The virus lies dormant in sensory nerve ganglia until it reactivates in the distribution of the affected ganglia. This results in a dermatomal eruption of a vesicular rash. In ophthalmology, particular attention is paid to rule out involvement of the eye resulting in keratitis, iritis, or acute retinal necrosis. Ocular involvement is greatest with V1/ophthalmic branch involvement, but may be seen with V2 distribution as well. In this particular patient, there was no evidence of the corneal involvement nor intraocular inflammation that can sometimes be seen with herpes zoster.
Of interest in this patient is the presence of ectropion secondary to a significant amount of localized induration and edema. This was secondary to suspected bacterial cellulitis superimposed on the affected area, as can often occur with zoster skin lesions. There was initial concern that scarring of the cheek could have resulted in permanent ectropion. However, prompt treatment with ocular lubrication, oral acyclovir for the zoster, and oral cephalexin (Keflex®) for the cellulitis resulted in resolution without corneal damage nor permanent ectropion (Figure 2). In some patients, however, this can be a permanent result.
| Same patient 1 week after treatment with acyclovir and cephalexin (Keflex). Note resolution of vesicles with remaining excoriated areas. Less ectropion is present, and this eventually resolved completely. |
|
Course: The patient did have some persisting pain and parasthesias in the V2 distribution even after resolution of the skin lesions. This pain was controlled with oral gabapentin (Neurontin). In close follow-up, the cornea never showed signs of involvement.
EPIDEMIOLOGY
|
OCULAR SIGNS
|
SYMPTOMS
|
TREATMENT (for isolated skin involvement)
|
Suggested citation format: Maassen J, Oetting T. Herpes Zoster Post-herpetic Neuralgia: 68-year-old male with decreased vision. EyeRounds.org. June 20, 2005; Available from: http://www.EyeRounds.org/cases/41-Herpes-Zoster-Post-Herpetic-Neuralgia.htm.

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.