Combined Hamartoma of the Retina and Retina Pigment Epithelium (CHRRPE)
Contributor: Eric Chin, MD and Brandon Menke
Photographer: Brice Critser, CRA
A 5-year-old male initially presented in 2004 complaining of decreased vision in the left eye for at least the prior six months. His parents denied any eye trauma. His birth history was unremarkable. His general health was also unremarkable.
Best corrected visual acuity at presentation was 20/25 in the right eye (OD) and 14/400 in the left eye (OS). Slit lamp examination was normal.
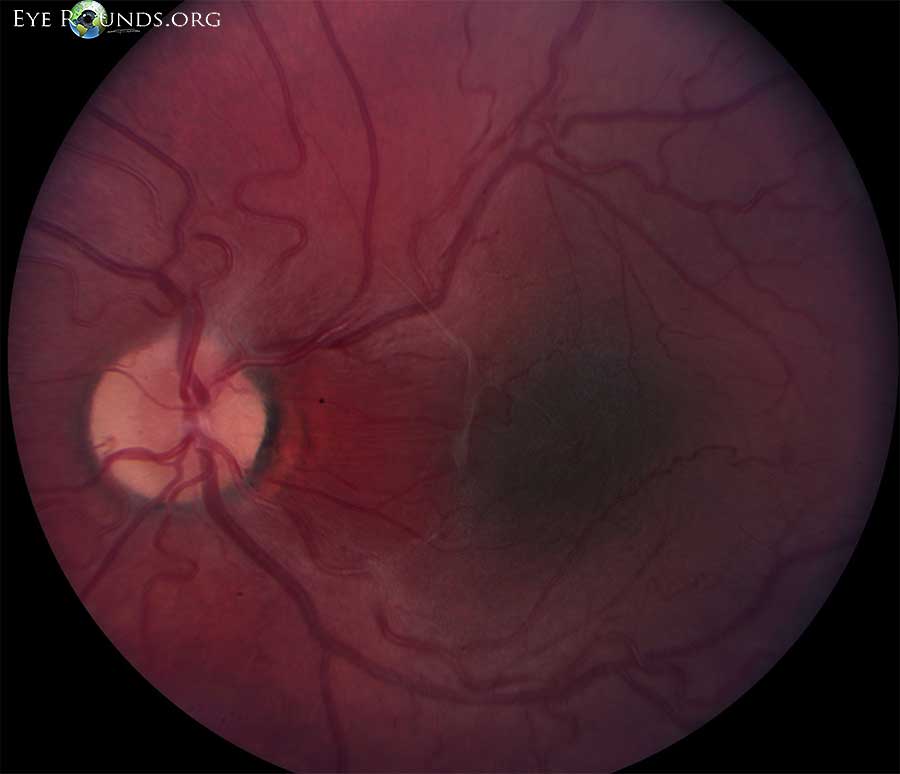
Figure 1. Left eye in 2004. At presentation, dilated fundus exam of the right eye was normal. In the left eye, there was a 5 x 5 x 1 mm area of slightly elevated retinal pigment epithelium (RPE) pigmentation with a surrounding area of more orange appearing RPE. The temporal arcades were distorted and displaced towards the center of the fovea. There was an epiretinal membrane over the nasal portion of the fovea, extending superiorly. There were fine retinal striae extending towards the optic nerve. There were no vitreous cells and the periphery was normal.
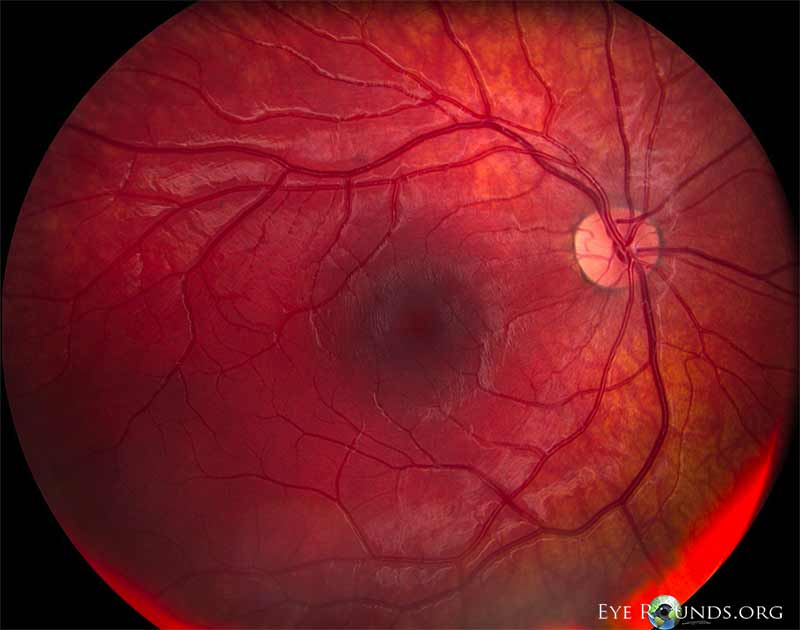
Figure 2. Right eye in 2006. In 2006, best corrected visual acuity was 20/15 OD and count fingers OS. There was a left exotropia and central scotoma OS. The peripheral fields were full OS, and confrontation fields were full OD.
Dilated fundus examination OD revealed a small cup with a cilioretinal artery. The discs, macula, vessels and periphery were normal.
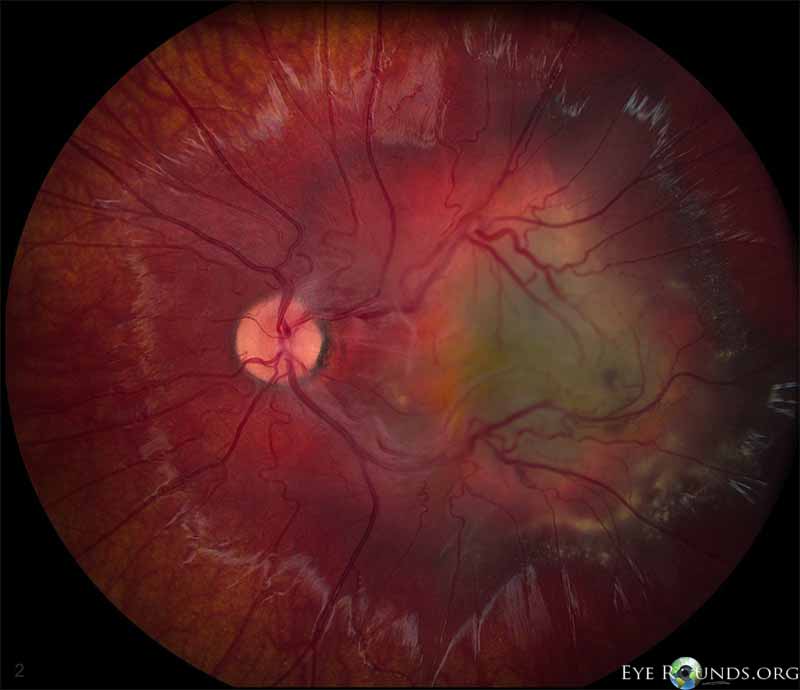
Figure 3. Left eye in 2006. In the left eye, the pigmented macular lesion appeared approximately the same size as was noted previously, but the surrounding orange colored ring appeared considerably more prominent. The retinal blood vessels were still dilated and tortuous, and they appeared to drain the central portion of the lesion, at least partially. There was an epiretinal membrane with more apparent traction on the retina. There was shallow subretinal fluid with some cystoid macular edema overlying the lesion, and there was subretinal lipid inferior to the lesion.
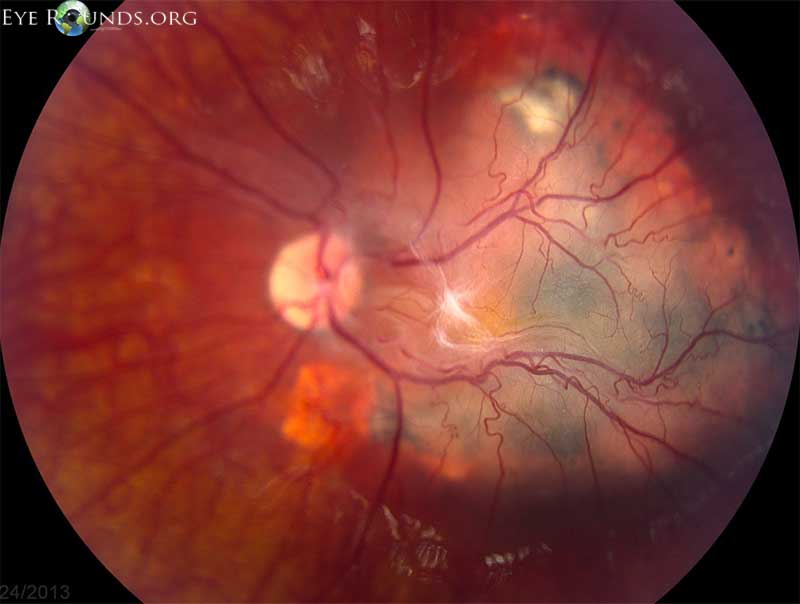
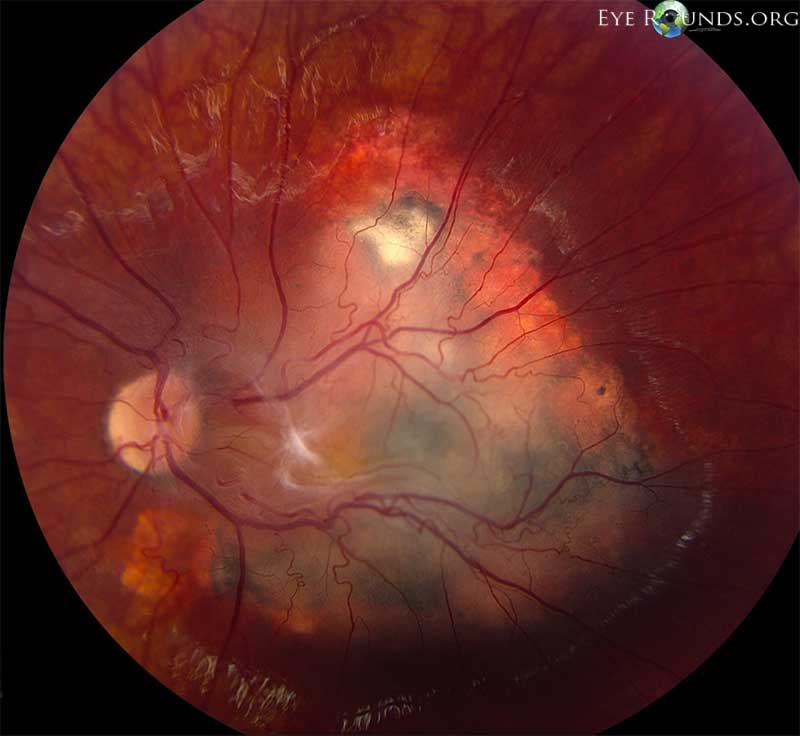
Figure 4. Left eye in 2013. In 2013 in the left eye, the variably pigmented macular RPE and retinal lesion had progressed and now measured 9 x 8 x 2.4 mm. The epiretinal membrane had also progressed. The arterioles and venules appeared to dive into the lesion temporal to fovea, but were now less dilated than previously.
Figure 5. Left eye in 2013. Same as figure 4, different angle and contrast.
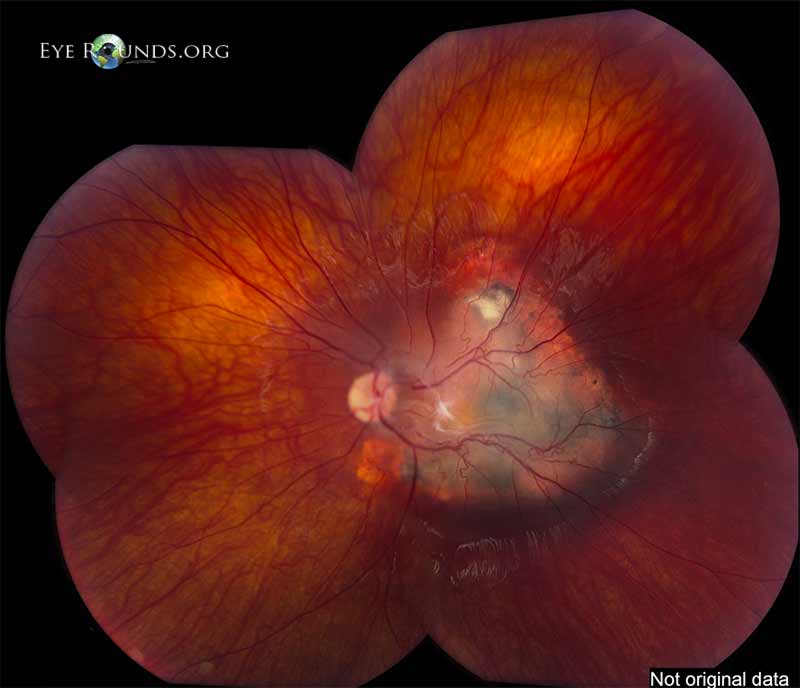
Figure 6. Left eye in 2013. Same figures 4 and 5, different angle and contrast – montage.
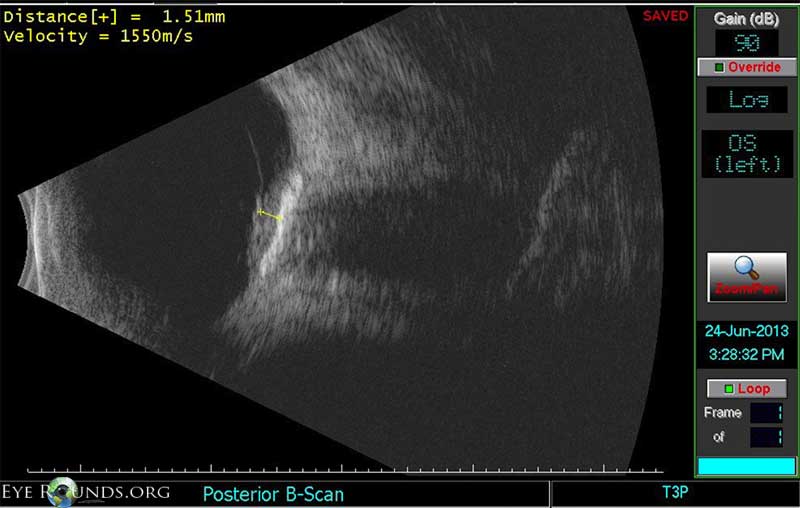
Figure 7. Echography in 2013. Echography of the left eye in 2013 revealed a lobular-shaped 2.5 mm (height) by 9.5 mm (base) medium-high-reflective lesion in the macula with a calcified plaque at the surface of the lesion.
Figure 8. OCT of right eye in 2013. Optical coherence tomography of the right eye was normal.
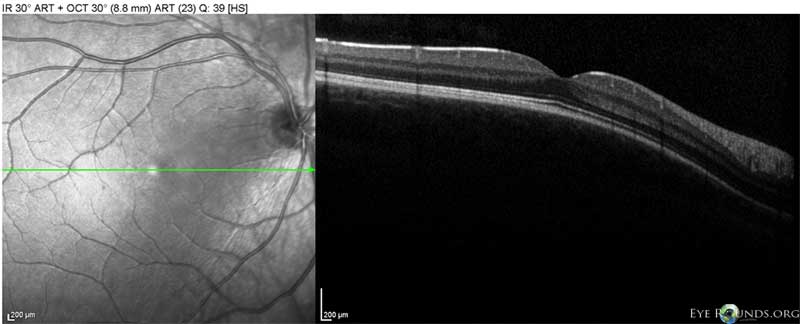
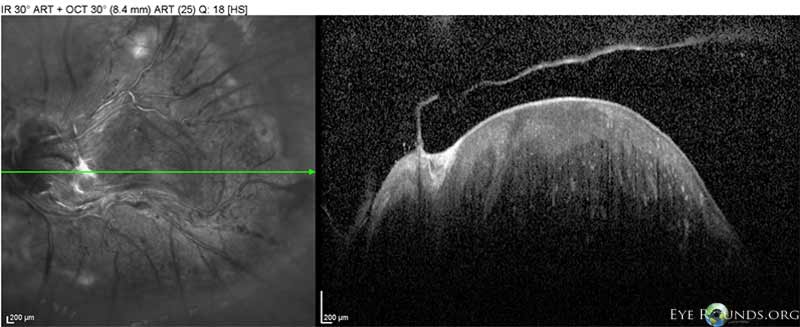
Figure 9. OCT left eye in 2013. Optical coherence tomography of the left eye in 2013 revealed a highly reflective elevated macular lesion with hyporeflective shadowing of the underlying tissue and obscuration of the normal retinal layers. There was also an epiretinal membrane and a stage 2 posterior vitreous detachment.
Discussion
- Combined hamartomas of the retina and retinal pigment epithelium (CHRRPE) are benign tumors that may cause significant vision loss depending on location.
- They are usually solitary and unilateral lesions located at the optic disc or posterior pole, and they may progress with time.
- CHRRPE are typically slightly elevated and have varying amounts of pigmentation, vascular tortuosity, and epiretinal membrane formation.
- Age, symptoms, and visual acuity are related to tumor location. Compared with extramacular lesions, macular lesions are associated with younger presentation (mean age 14.2 months old versus 9.5 months old), strabismus (25% versus 31%), and decreased visual acuity (37% versus 43%), and visual acuity ≤20/200 (25% versus 69%).[1]
- Other findings include vitreous hemorrhage, pre-retinal neovascularization peripheral to the hamartoma, choroidal neovascularization at the margin of the lesion, macular hole, and peripheral hole formation.
- Most patients do not have systemic disease, however, numerous reports describe an association with neurofibromatosis type 1 and 2.
Differential Diagnosis
- Choroidal nevus
- Choroidal melanoma
- Melanocytoma
- Morning glory disc anomaly
- RPE adenoma
- RPE adenocarcinoma
- Retinoblastoma
Reference
1. Shields CL, Thangappan A, Hartzell K, et al. Combined hamartoma of the retina and retinal pigment epithelium in 77 consecutive patients. Ophthalmology 2008;115:2246-2252.

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.