A 33-year-old male with history of bilateral aphakia s/p intracapsular cataract extraction (ICCE) of dislocated lenses at age 13 presented with recurrent episodes of floaters and blurred vision in the left eye over the past year. These episodes lasted anywhere between one hour and half a day, and were initially once per month but had been increasing in frequency and were occurring at least twice a week at time of initial presentation. He was found to have vitreous hemorrhage on examination by his local eye doctor and was referred to the University of Iowa for further evaluation.
Past Ocular History: Aphakia in both eyes (OU) s/p ICCE for dislocated lenses at the age of 13
Past Medical History:
Medications: metoprolol
Allergies: None
Family History: Marfan’s syndrome in his father and son, both have dislocated lenses
Social History: non-contributory
Review of systems: non-contributory
Pupils: Reactive to light in each eye from 4 mm in the dark to 3 mm in the light. No relative afferent pupillary defect (RAPD).
Extraocular movements: Full OU
Confrontation visual fields: Full OU
Downslanting palpebral fissures and malar hypoplasia
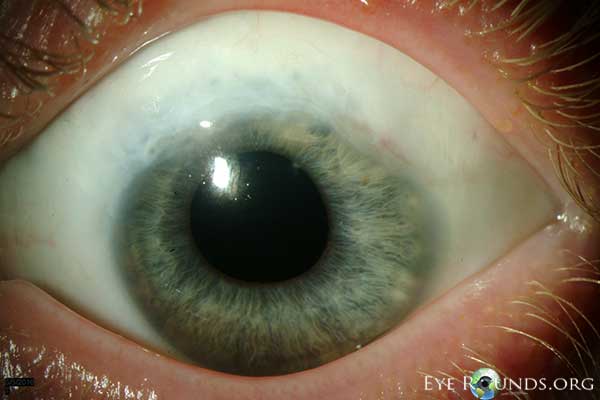 |
The optic nerves appeared healthy with a 0.3 cup-to-disc ratio. The maculae were normal OU. The vessels were normal. There was patches of lattice inferiorly OD and vitreous hemorrhage inferiorly OS obscuring the view of the inferotemporal retina.
Because of the concern for a possible tear and rebleeding from bridging retinal vessels underneath the vitreous hemorrhage inferotemporally OS, the patient underwent cryotherapy OS to the inferotemporal retina. One month later, he continued to have recurrent vitreous hemorrhages OS.
The patient was told to come in during an episode of bleeding for examination while he was symptomatic. During his next episode, he was found to have bleeding into the anterior chamber from a posterior wound gap within the old cataract wound OS. On gonioscopy, the abnormal vessels were seen superotemporally within the prior ICCE wound and deemed the source of bleeding (Figure 2).
 |
Diagnosis: Recurrent bleeding from cataract wound neovascularization (Swan syndrome)
Recurrent intraocular bleeding from a prior cataract wound was first described by Swan in 1973 (Swan, 1973). Since that time, there has been a handful of case reports and case series describing this entity (Banitt et al., 2009; Bene et al., 1989; Benson et al., 1978; Jarstad and Hardwig, 1987; Watzke, 1974, 1980) . Intraocular hemorrhage can occur months to years after uncomplicated cataract surgery involving a scleral incision due to wound neovascularization (Bene et al., 1989). Following intracapsular cataract extraction, bleeding from these abnormal blood vessels can result in hyphema and/or vitreous hemorrhage in patients with aphakia, whereas following extracapsular cataract extraction, bleeding from wound neovascularization typically results in hyphema alone, unless the posterior capsule or zonules are compromised.
Patients generally present with intermittent visual loss generally lasting on the order of hours, but can last days. Intraocular hemorrhages may be precipitated by minor trauma or straining, but can be completely spontaneous. In rare cases, the visual loss can be accompanied by painful hemolytic glaucoma or angle closure glaucoma (Bene et al., 1989). Symptoms are typically unilateral, but bilateral cases have been reported (Banitt et al., 2009) .
The abnormal vascularization appears to arise from an extension of episcleral vessels into the cataract wound, likely due to poor wound apposition (Bene et al., 1989; Jarstad and Hardwig, 1987; Swan, 1973) . Postmortem studies suggest focal abnormal vascularization of the cataract wound is not a rare sequelae of cataract surgery involving scleral incisions (Jarstad and Hardwig, 1987). However, neovascularization of the wound has not been reported in clear corneal incisions (Banitt et al., 2009) .
A careful dilated retinal examination must be performed to rule out vitreous traction, retinal tear, or retinal vascular disease. Gonioscopy will ultimately provide the diagnosis, which reveals wound neovascularization at the prior scleral incision. Rocking or manipulation of the gonioscopy lens may provoke bleeding and aid in the diagnosis (Watzke, 1974). Gonioscopy fluorescein angiography can also be used to establish the diagnosis (Watzke, 1974).
The first line treatment is focal argon laser photocoagulation through a gonioscopy lens. Generally, short pulses with high intensity are used to blanch the abnormal blood vessels (Bene et al., 1989). Retreatment may be necessary because episcleral vessels often regrow leading to recurrences (Watzke, 1980). If laser photocoagulation is unsuccessful, the wound can be surgically reopened and treated with direct diathermy, cryopexy, or surgical excision of the blood vessels (Swan, 1973; Watzke, 1980) . We successfully treated our patient with limbal sutures across the cataract wound (see below).
Because abnormal neovascularization of the wound does not occur in clear corneal incision cataract extraction, the incidence of Swan syndrome will likely be reduced in the future. Nevertheless, keeping this increasingly rare entity in mind can be helpful in diagnosing late intraocular hemorrhages in patients that have previously undergone intraocular surgeries involving scleral incisions.
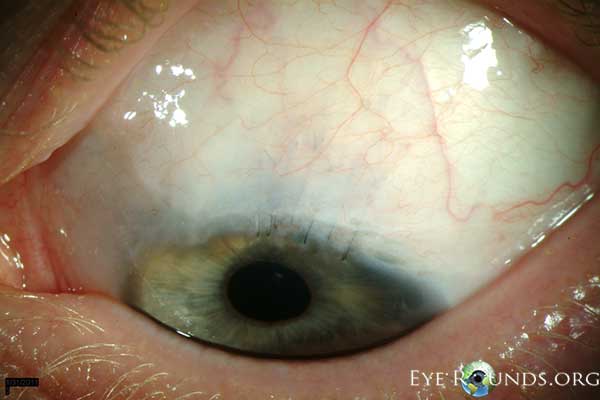
The patient underwent argon laser photocoagulation through a gonioscopy lens, but had minimal improvement in his symptoms. He then underwent wound revision with cautery to the limbal vessels and had a mild improvement. Because he continued to have significant intraocular hemorrhages, we placed multiple 10-0 nylon limbal sutures across the gap within the cataract wound to help approximate the wound and prevent recurrences of bleeding (Figure 3). Although this created a large degree of astigmatism, the procedure successfully stopped the recurrent hemorrhages. After two years of quiescence, he recently developed a few episodes of recurrent bleeding, but much less frequently than his initial presentation. We are currently observing given the infrequency of the hemorrhages.
 |
Epidemiology:
|
Symptoms:
|
Signs:
|
Treatment
|
Chen JJ, Kwon YH. Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome). EyeRounds.org. August 6, 2012; Available from: https://eyerounds.org/cases/153-Swan-Syndrome.htm

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.