History of Present Illness: The patient was diagnosed as having Duane syndrome at the age of 10 months and has been followed by a local ophthalmologist since then. His present concern is globe retraction in the left eye on right gaze and asymmetry of the palpebral fissures on side gazes. There is no history of diplopia in primary gaze.
Past Ocular History: No history of ocular surgeries. History of patching right eye in childhood.
Medical History: Unremarkable
Medications: None
Family History: Noncontributory
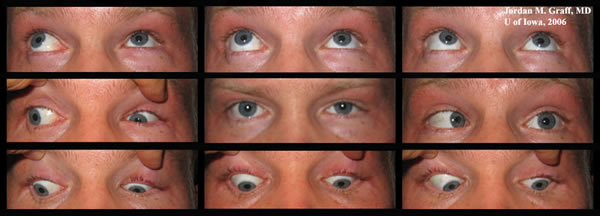 |
Course: The patient’s symptoms and motility examination are consistent with Type III Duane retraction syndrome. The patient had excellent visual acuity with no strabismus in primary position and no abnormal head position. His main concern was globe retraction with enophthalmos and psedo-ptosis in attempted right gaze. Globe retraction and field of single binocular vision can be improved in patients with Duane retraction syndrome through surgical intervention. One could consider inactivation of lateral rectus by disinserting the muscle with reattachment to the orbital periosteum, accompanied by augmented vertical muscle transposition. However, we advised the patient against this procedure in his particular case since his ocular alignment for two main reasons: this patient is orthophoric in primary position and he had no anomalous head position.
Discussion: Duane retraction syndrome is a congenital ocular motor disorder characterized by limited abduction and/or adduction accompanied by palpebral fissure narrowing and globe retraction on attempted adduction. Although this syndrome was described in isolated case reports by Sinclair, Bahr, Stilling and Turk; Duane was the first to describe a case series of 54 cases (Duane), summarizing all findings, and offering theories on pathogenesis and treatment.
Huber (Huber, et al) compartmentalized Duane syndrome into three types based on clinical findings and electromyographic recordings. Duane Type 1 consists of limited or absent abduction with relatively normal adduction, Duane type II consists of limited or absent adduction with relatively normal abduction and Duane type III is characterized by both limited abduction and adduction. The evidence from neuropathological, neuroradiological and neurophysiological studies suggests that the etiology of Duane syndrome is a neurogenic brainstem ocular motor dysfunction resulting from faulty embryogenesis. Most of the studies have suggested an absence of cranial nerve VI and/or its nucleus with aberrant innervation of the lateral rectus by a branch of the third cranial nerve. Duane syndrome has now been classified as a subset of congenital cranial dysinnervation disorders. Long-standing misalignment of the eye can result in secondary changes of the extraocular muscles. Excess innervation to the muscle may cause overaction and globe immobility. Some of these changes are: superior rectus contracture from upshoot, medial rectus contractures from large esotropia, or stretched-out medial rectus in long-standing exotropia.
Some of the important considerations in management of a patient with Duane syndrome are misalignment in primary position, abnormal head position, and severity of cocontraction, upshoot/downshoot and secondary muscle changes. Evaluation of refractive error and its correction is essential as amblyopia in Duane syndrome is mostly refractive in nature.
Surgical goals in Duane syndrome include decreasing or eliminating the anomalous head position, centering and expanding single binocular visual fields; and increasing abduction while preserving adduction. The surgical management in a case of Duane syndrome should be tailored according to the severity of the problem and specific needs of the patient. The treatment options and realistic expectations should be discussed with the patient and the family in detail. The various surgeries that have been described are unilateral or bilateral medial rectus recession, horizontal transposition of vertical recti with or without medial rectus recession, vertical rectus transposition with lateral augmentation and partial rectus augmented transposition. Upshoots and downshoots have been improved by surgical techniques such as large recession of lateral rectus, combined lateral and medial rectus recession or Y- splitting with recession of the lateral rectus. Severe co-contraction, globe retraction and limitation to adduction may improve if the lateral rectus is maximally recessed or its insertion is inactivated from the globe along with augmented vertical rectus transposition.
Diagnosis: Duane Retraction Syndrome, Type III (Duane's Syndrome, The Duane Syndrome, Congenital retraction syndrome)
EPIDEMIOLOGY
|
SIGNS
|
SYMPTOMSThe syndrome is almost always diagnosed early in life with the parents typically noticing the limitation to versions
|
TREATMENT
|
Bhola R, Graff JM: Duane Retraction Syndrome: 31-year-old Male With Globe Retraction. Eyerounds.org. June 1, 2006. [cited -today's date-]; Available from: http://www.EyeRounds.org/cases/56-Duanes-Retraction-Syndrome.htm.

Ophthalmic Atlas Images by EyeRounds.org, The University of Iowa are licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License.