
Section 12-A: Using Glaucoma Medications Regularly
The Patient-Doctor Relationship
The most important controllable factor in glaucoma management is adherence to prescribed medications. A good patient-doctor relationship fosters knowledge of the disease process and greater likelihood of adhering with a recommended regimen. The more patients know about their disease process, the more likely they are to adhere to treatment. It is the eye care providers’ responsibility to inform patients of their diagnosis and its implications. A common misconception is that blindness is the inevitable result of glaucoma. While there is a possibility of blindness in glaucoma, it is not necessarily inevitable. With proper diagnosis and early intervention, most patients retain functional vision with limited visual disability. Asking the doctor questions and better understanding of the disease are part of effective treatment.
Understanding Goals of Treatment
Since glaucoma is a chronic condition, once treatment is initiated it is often continued throughout a patient’s lifetime. The goal of medications is to prevent a further decline of vision by lowering the intraocular pressure (IOP). This goal is sometimes not obvious to patients because instead of restoring previously lost vision, it aims toward preventing further vision loss. The presumed lack of direct benefit hinders adherence with glaucoma medications. When patients see no direct benefit from taking medications, they may be less inclined to take them as prescribed. In addition, the vision loss from glaucoma tends to occur slowly over time and there are usually no acute symptoms. Patients do not notice the vision loss that occurs over a long time period and fail to see this as being a result of not taking their glaucoma medications. Although the immediate benefit is not obvious, it is important to realize that taking daily eye drops is decreasing the likelihood of vision loss from glaucoma.
Worsening Glaucoma with Missed Doses
Missed doses of medications can cause vision loss as much as not taking glaucoma medications altogether. The fluctuations in IOP can be equally detrimental to the optic nerve. A study which used electronically monitored medication bottles revealed that only 83% of timolol doses were taken as prescribed. The IOP measured the day of the exam can be misleading since most patients take their eye medications shortly prior to the examination. Unfortunately, there is no available physiologic parameter which allows the eye doctor to know what the average IOP has been between visits. Glaucoma can worsen when doses are repeatedly missed despite a good measurement at the doctor’s office. The fluctuations of IOP can be detrimental to the optic nerve.
A Team Approach to Battling Glaucoma
The treatment of glaucoma is a battle which must be fought by both the eye doctor and patient. It is very difficult, if not impossible, for an eye doctor to control glaucoma without the full participation of the patient. It is the patient who is responsible for the day-to-day treatment of glaucoma. The patient should be aware of the benefits and side effects of the recommended medications as well as the disease itself. A well-informed patient is more likely to adhere to a long-term medical treatment of glaucoma.
12-B: Adherence to Glaucoma Medications
Many studies have tried to evaluate the level of adherence in patients and the risk factors for nonadherence. In general, 13.4% to 60% of patients have reported their non-adherence when asked. Numerous factors have been evaluated to determine what affects adherence. Age, race, and gender have not been found to be contributing factors. Others are contributory and discussed below.
12-B(1): Factors Affecting Adherence
Forgetfulness. Many patients report forgetfulness as one of the major reasons that they are not 100% adherent with their glaucoma medications. It is often difficult to incorporate a new drug regimen into one’s lifestyle.
Physical Limitations. Those with physical limitations, such as severe arthritis or significant visual disability, may have problems self-administering medications. Family or caregivers can help treat glaucoma by accompanying the patient to appointments, understanding the disease, and learning how to administer eye drops if necessary.
Misunderstanding the Disease and Its Treatment. This factor is easily corrected by gathering information about the disease process. Information on glaucoma is readily available at your eye doctor’s office, the library, book stores, and the internet. These available resources are inexpensive and easily obtained.
Multiple Doses Per Day. The number of doses per day and number of medications can also affect adherence. The more doses or medications prescribed, the less likely that there will be perfect adherence. Instilling numerous doses or medications can adversely affect a patient’s lifestyle. It is difficult to remember multiple drops and take time to administer eye drops throughout the day. The more frequently this occurs, the more likely there will be missed doses. Given the time necessary and other methods involved with ensuring proper glaucoma medications, it is easy to see why patients prefer once daily-dosed eye drops. The following eye drops are administered once daily: Xalatan, Travatan, Lumigan, Timolol XE, Istalol.
Multiple Medications. One can improve adherence by minimizing the dosage and total number of medications that are still effective. Patients should be on the least number of eye drops necessary with the least dosing per day to control their glaucoma. Written instructions from the doctor’s office are a good reminder to be used at home, particularly for those on multiple systemic medications for other diseases. Combination eye drops [e.g., Cosopt (timolol/dorzolamide)] also exist which minimizes the number of eye drop bottles.
Difficulty Administering Medications. Eye drop delivery aids are available for people who have physical difficulty administering their eye medications. The bottle can be placed in these devices, and the device allows the patient to easily squeeze the bottle in the correct position over the eye. One eye medication, Travatan, offers an aid which electronically monitors doses and offers reminders when doses are due (Figure 12-1). This aid allows providers to download the information to see how adherent a patient has been since their last visit.
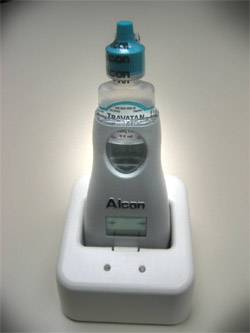
Figure 12-1. The Travatan Dosing Aid (Alcon, Ft Worth, TX) reminds patients when doses are due. It also allows the eye doctor to download information about the doses taken and their timing.
Intolerable Side Effects. In general, topical glaucoma eye drops are well-tolerated, especially with the newer generation of medications. Nevertheless, some people can experience untoward side effects. The various medications and the side effects are numerous and have been discussed previously (see Chapter 7).
High Cost of Medications. Patients are sometimes willing to pay more for medications which increase convenience and cause minimal side effects. Others are constrained by the cost, especially when they are taking other medications for systemic diseases.
12-B(2): Measures to Improve Adherence to Glaucoma Medications.
Understand the Disease and Its Treatment. Patients are encouraged to ask questions about their diagnosis and understand the rationale behind its treatment. Obtain information on the disease from the prescribing provider, books, and online glaucoma sites
Prescribing Least Number of Medications/Doses. Adherence can be improved by using the least number of medications and least number of doses per day to control glaucoma
Minimize Untoward Side Effects. Report adverse side effects from eye drops. Understand the expected side effects and identify which ones are not transient. Some medications may cause slight redness upon initial instillation of the drop which improves with time.
Get Written Instructions. Written instructions are helpful for the patient to recall the exact medical regimen prescribed by the eye doctor (Figure 12-2). Relying only on verbal instructions often leads to mistakes in administration of medications. It is difficult for the patient to remember all verbal instructions when there is so much information given during a clinic visit.

Figure 12-2a. A medication instruction sheet is a helpful reminder to take medications as exactly prescribed

Figure 12-2b. Guidelines for Using Medications
Use Colors to Identify Correct Medications. It is important to know what medications are prescribed, what they do, and how to correctly identify them. The bottles cap color provides a helpful reminder of what each bottle contains (see Chapter 7, Table 7-2).
Practice Administering Medications in the Clinic. Patients are encouraged to practice administering eye drops under the supervision of their eye doctor. This allows the eye doctor to see how well a patient is instilling their medications. It also reassures the patient that their instillation technique is correct.
Time Doses with Scheduled Activities. Dose eye drops with scheduled activities. Patients can often incorporate their medication in the morning, with meals, and at bedtime. Linking the eye drop with an activity, such as brushing teeth or taking other oral medications, is helpful.
Obtain Help from Family/Caregivers. Enlisting the help of others may be necessary for those who are unable to comprehend or self-administer eye drops. Family/caregivers’ understanding of the disease and its treatment is key to improving adherence to a prescribed drug regimen.
Perform Punctal Occlusion or Eyelid Closure. It is recommended that patients wait 10 minutes between medications to allow better absorption of each medication. If 3 eye drops have been prescribed, there would be 20 minutes of waiting time per dose. For example, if there are 3 medications that need to be taken twice daily each, more than 40 minutes of time is necessary to administer these medications each day. It is easy to see how an increase in the number of medications causes a decrease in adherence. Another method of improving absorption of eye drops is to use punctual occlusion. This maneuver allows the eye medication to absorb more effectively by obstructing the outflow from the eye. It is performed by placing digital pressure over the lower eyelid puncta by the nose (see Chapter 7, Figure 7-4, 7-5).
Use Eye Drop Delivery Aids If Necessary. Eye drop delivery aids could be useful in some patients. For those with arthritis or severe vision loss, it may be useful (Figure 12-3)
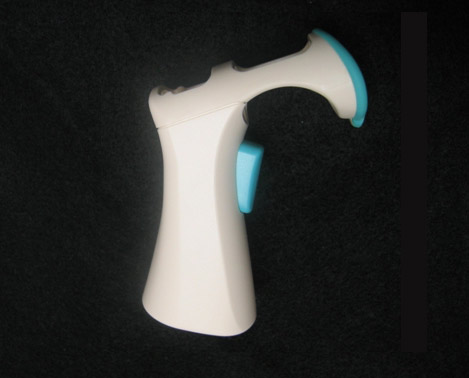
Figure 12-3. An eyedrop dispenser for Xalatan (Xal-Ease, Pfizer, NY, NY) can help those who have difficulty administering Xalatan eye drop.
Checking on Prescription Refills to Determine Adherence Level. Patients and eye doctors can check on the number of refills within a certain time period. This gives a general estimation to see if the usage seems on track.
Generics and Understanding Available Resources to Decrease Cost Generic glaucoma medications are available which helps to defray some of the cost.
The Glaucoma Research Foundation provides information on financial aid and programs that assist patients with obtaining their glaucoma medications.
12-C: Low Vision Aids
If glaucoma is undiagnosed or poorly controlled, it may result in varying degrees of visual disability. Once vision loss occurs from glaucoma, it cannot be regained. If the loss is mild, the patient may not experience any limitation in their daily activities. If moderate, there may be some visual impairment. In advanced cases, functional vision can be severely compromised to the point of legal blindness. It is, therefore, important to have periodic scheduled monitoring for glaucoma with good adherence to a prescribed drug regimen. This can minimize the visual decline resulting from glaucoma.
When functional visual disability exists, evaluation by a Vision Rehabilitation Specialist is important. A vision rehabilitation specialist is an eye doctor trained in providing low vision evaluations and presenting devices which may assist patients in their daily activities. The purpose of a Vision Rehabilitation Specialist is to improve individual’s activities of daily living (ADLs) so that the disability’s effects are minimized. These specialists can assess a person’s needs within both home and occupational settings and provide recommendations to improve their level of functioning within these areas. A consultation may provide instruction on the optimal eyeglass prescription (near and far), lighting for various tasks, and an assessment of driving. Various low vision aids may be beneficial, including high prescription reading glasses, filtered lenses, handheld and free-standing magnifiers, talking clocks/books and other appliances, large print materials, electronic reading machines, telescopes, closed circuit televisions/video magnifiers, computer access technology, and devices for braille. These aids allow patients to optimize their functioning in both home and occupational settings. For example, adequate task lighting and prescription strengths for reading may be evaluated so that reading is easier and more enjoyable. Filtered lenses can help with light sensitivity or problems with glare. Both handheld and free-standing magnifiers are helpful for patients who require increased magnification for better reading. They come in different strengths. Handheld magnifiers have the benefit of being portable but are bothersome for those with hand tremors. Free-standing magnifiers are more useful in these cases but have the disadvantage of not being easily portable. Talking clocks/books and other appliances are also helpful for visually disabled persons. They allow people to rely on their hearing to obtain information. Large print books are helpful for those who need extra magnification for easier reading. These are available in book stores and libraries. Closed circuit TVs/video magnifiers have a camera which magnifies images that are then relayed to a monitor for viewing. This is useful for reading material such as newspapers or for important activities such as reading bills or signing checks. A Low Vision evaluation aims toward improving patients’ lifestyles by analyzing their needs and providing the means and methods to meet them.
12-D: Minimizing the Impact of Glaucoma on Lifestyle
A chronic disease requires chronic treatment. The diagnosis of glaucoma often means a lifetime of ophthalmic exams and treatment. Chronic treatment and monitoring should be incorporated into one’s life with minimal strain or stress to the patient. One of the major factors affecting how likely a patient will be adherent with medications is the impact of glaucoma treatment on a person’s lifestyle. Physically active patients would prefer not to have continual disruptions in their day to administer medications. It is important to minimize the number of medications/doses per day to adequately control glaucoma. The number of prescribed medications increases if glaucoma is uncontrolled with existing medications. Doses per day depend on the prescribed medication. Once-daily dosed medications help minimize the time requirement for administration.
Incorporating medications into a daily routine helps prevent missed doses. Once a routine is established, there is less of a chance of forgetting medications. Until a routine is established and memorized, it is helpful to have written instructions to follow. This eliminates dosing the incorrect eye or using the wrong number of doses.
When glaucoma surgery is warranted, the type of procedure chosen can be influenced by lifestyle choices. Discuss your activities with your doctor to guide surgical treatment. Input from the patient helps to maximize surgical success.
Cost becomes an issue with using glaucoma medications. The average cost per month can be significant depending on the number of medications used. Generic brands are available for some of the eye drops which can decrease their cost substantially. A prescription health plan and other benefits (e.g., veterans’ benefits) also help to defray the cost of these prescription medications. Comparing costs of medications online is another method of finding the most economical alternatives. Using drug delivery aids can prevent wasted doses by effectively delivering the medications to the eye. A discussion with your provider helps coordinate a plan for the most effective and least costly drug regimen.
Take advantage of low vision aids and existing benefits. Computer monitor settings can be changed to increase font size and appearance of the screen for advanced visual loss. In the United States, a person who has significant vision loss or is legally blind (best corrected vision less than 20/200 or visual field < 20º in the better eye) may qualify for Social Security or Supplemental Security Income (SSI) benefits (http://www.ssa.gov/) or tax benefits (http://www.irs.gov/). Directory assistance and other benefits may be available depending on the state of residence. The Library of Congress (www.loc.gov/nls) also provides free library services for the visually impaired and physically disabled. Veterans may also qualify for benefit through their Veterans Administration (http://www.va.gov/).
12-E: Glaucoma Societies and Organizations
Numerous glaucoma resources are available to patients and eye doctors alike. The following is a list of the larger national organizations. They each provide links to other organizations and support groups.
The American Academy of Ophthalmology (www.aao.org) is the national organization for ophthalmologists. Its membership and resources are extensive. A special Patient section is provided which answers many questions about glaucoma. In addition to providing information on various Eye Health Topics, it contains helpful sections regarding glaucoma.
The American Glaucoma Society (www.glaucomaweb.org) is a nationally recognized society whose members are practicing glaucoma specialists. It also provides patients with basic information about glaucoma and its treatment. It is a nice resource for patients who are looking for a glaucoma specialist in their geographical location.
The Glaucoma Foundation (http://www.glaucomafoundation.org/) is a not-for-profit organization which provides patients information about their diagnosis and treatment and provides funding for glaucoma research. Information is presented in an easy to understand format.
The Glaucoma Research Foundation (www.glaucoma.org) provides funding for glaucoma research. The Foundation provides access to support services and discusses issues regarding financial assistance with glaucoma medications.
Research to Prevent Blindness (http://www.rpbusa.org/) is a non-government organization which provides generous funding for eye research. Basic concepts of glaucoma are discussed and presented.
Several international groups exist. The Association of International Glaucoma Societies, of which the American Glaucoma Society is a regional member, is an international organization which facilitates collaboration among many glaucoma societies throughout the world. It attempts to distribute and consolidate information regarding the standard practice of glaucoma. The Association of International Glaucoma Patient Organizations arose from The Association of International Glaucoma Societies and provides patients with regional support groups and references regarding patient education.
Finally this entire book, A Patient’s Guide to Glaucoma, is also available for purchase as a softcover book at Amazon.com.
Chapter 12. References
Busche S, Gramer E. [Improved eyedrop administration and compliance in glaucoma patients. A clinical study]. Klin Monatsbl Augenheilkd. 1997 Oct;211(4):257-62.
Gurwitz JH, Glynn RJ, Monane M, Everitt DE, Gilden D, Smith N, Avorn J. Treatment for glaucoma: adherence by the elderly. Am J Public Health. 1993 May;83(5):711-6.
Kass MA, Gordon M, Morley RE Jr, Meltzer DW, Goldberg JJ. Compliance with topical timolol treatment. Am J Ophthalmol. 1987 Feb 15;103(2):188-93.
Kosoko O, Quigley HA, Vitale S, Enger C, Kerrigan L, Tielsch JM. Risk factors for noncompliance with glaucoma follow-up visits in a residents’ eye clinic. Ophthalmology. 1998 Nov;105(11):2105-11.
Muir KW, Santiago-Turia C, Stinnett SS, Herndon LW, Allingham RR, Challa P, Lee PP. Health literacy and adherence to glaucoma therapy. Am J Ophthalmol. 2006 Aug;142(2):223-6.
Patel SC, Spaeth GL. Compliance in patients prescribed eyedrops for glaucoma. Ophthalmic Surg. 1995 May-Jun;26(3):233-6.
Sleath B, Robin AL, Covert D, Byrd JE, Tudor G, Svarstad B. Patient-reported behavior and problems in using glaucoma medications. Ophthalmology. 2006 Mar;113(3):431-6.
Vold SD, Riggs WL, Jackimiec J. Cost analysis of glaucoma medications: a 3-year review. J Glaucoma. 2002 Aug;11(4):354-8.